Information Research, Vol. 5 No. 3, April 2000


Information Research, Vol. 5 No. 3, April 2000 | ||||
 |
 |
|||
Les Smith |
and |
Hugh Preston |
Clatterbridge Centre for Oncology | Department of Information and Library Studies |
The UK National Health Service’s strategic switch-back is well documented and each centrally originated change results in various attempts to record the repercussions and predict the outcomes. The most recent shift is embodied in the Department of Health’s information strategy, Information for health published in September 1998. This document provides the context for an examination of the issue of developing an Information Management and Technology (IM&T) strategy at the local level within the changing national requirements for NHS information management. The particular pressures on an individual unit and the need to react to them alongside the requirements of the national strategy are the subjects of this article. The case detailed is that of Clatterbridge Centre for Oncology (CCO) on Merseyside, the second largest centre of its type in the UK. Its initial investigation of information needs preceded the publication of the national strategy and its implementation straddled the timescale devised by the NHS Information Authority. The inevitable incompatibility between timescales for the local and the national developments is examined within the case. The work of the new NHS Information Authority and its supporting guidance in its Circular, Information for Health: Initial Local Implementation Strategies, is evaluated as a tool in aligning local and national strategy. Information Managers in other centrally governed organisations within the public sector and large corporations are often alert to similar issues.
The British Medical Association produced a press release immediately after the publication of the Information for health strategy which stated the Association’s confidence in the focus of the strategy.
"The whole focus of NHS IT has been hauled away from management and finance and towards patient care." (Lajca 1999)
Nevertheless, the focus on direct patient care and clinical priorities does not deny the need to meet managers’ requirements for information. Just as corporate information managers often struggle to cope with the remote requirements of central head-quarters (Teo, T.S.H. and Ang, J.S.K. 1999; Ma et al 1999), those within the health sector have to meet the demands of central government as well as regional and local management. The UK National Health Service’s (NHS) strategic switch-back is well documented and each centrally originated change results in various attempts to record the repercussions and predict the outcomes. The speculative commentaries of professional journals such as Health Service Journal are punctuated by periodic reviews by analysts of longitudinal change. The implications for IM&T are frequently considered alongside issues of direct care. The most recent shift is embodied in the Department of Health’s information strategy, Information for health published in September 1998. This document provides the context for an examination of the issue of developing an IM&T strategy at the local level within the changing national requirements for NHS information management. The case detailed in this paper is that of Clatterbridge Centre for Oncology (CCO) on Merseyside, the second largest centre of its type in the UK. Its implementation of a new principal information support system (to replace one installed in 1992) straddled the development of the new national strategy. This paper draws on this experience to assess the significance for NHS institutions of national initiatives on local plans for information systems. The inevitable incompatibility between timescales for local and national developments is examined within the case. The work of the new NHS Information Authority and its supporting guidance in its Circular, Information for Health: Initial Local Implementation Strategies is evaluated as a tool in aligning local and national strategy.
As an acute provider, CCO has carefully developed an IM&T strategy based primarily on local needs but remaining in accordance with the five basic principles set out by the NHS Information Management Group in 1992. Development of the CCO strategy has more recently had to incorporate the changes brought about by the White Paper of 1997 which introduced the principle of clinical governance. Within cancer care, all strategies for the provision of services have additionally had to incorporate the requirements of the Calman/Hine initiatives of 1995. The new national IM&T strategy, Information for Health, has resulted in some caution at the local level since IM&T managers have not wished to implement local strategic policies without confidence in their conformance to national requirements. The delay in publication exacerbated this situation. At CCO one outcome of this was wariness in replacing the principal information support system that was not meeting current information requirements. However, development of the IM&T strategy continued, with an objective to facilitate system replacement. The new national strategy, published in September 1998 closely matches the CCO strategy in terms of aims and means of information provision. CCO is therefore well placed to implement its strategy and achieve the balance that is needed but difficult to accomplish. The close match between local needs and national strategy was unexpected due to the problems faced by cancer units in incorporating previous standards developed in accordance with the requirements of general medicine. Related research has highlighted the difficulties met in keeping in step with national policy whilst still maintaining local benefits (Bowns et al 1999).
The NHS information strategy, Information for Health, published in September 1998 provides a framework for IM&T (Burns 1998). This focuses on the NHS as a whole, but predictably aims to ensure strategic implementation at primary care level first. This is inevitable, given The New NHS White Paper’s commitment to modernisation of GP systems (Mitchell 1998). The strategy states the case for electronic patient and electronic health records (EPR and EHR) and links this to their importance in supporting strategic ‘strands’. These include developing clinical information standards and improving use of NHSnet. From the local point of view an implementation timescale is specified in accordance with the ten year modernisation programme identified in The New NHS.
Despite the primary care priorities, standards for EPR and EHR will equally apply to acute providers such as cancer centres. They will inevitably influence local IM&T strategies through their technical standards. For CCO, the absence of an IM&T strategy since becoming a Trust in 1992 has hampered the development of information resources, but now enables systems development to be in accordance with the national strategy.
If the IM&T manager is to be effective, a balance between local information needs and national strategies must be established. For all elements of the NHS this is seldom capable of being achieved within the span of control of an individual manager, nor the operating unit in which the manager works. The ability to work within relatively definable boundaries does not exist to the extent that a manager in the commercial sector may experience. For a Trust such as the case of this study which is within a specialist environment, the broader NHS objectives are still of great significance. However, the Trust’s performance in comparative terms is less likely to be often under the microscope of public scrutiny. Government initiatives that relate to the oncology specialism itself are of additional significance. The issue of implementing the new information strategy alone is broadly addressed within the Information for health strategy document. The Information Policy Unit of the NHS Executive has also produced published guidance. This has been supported by input to various forums for examination of the issues from the point of view of information specialists within the NHS. Opportunities have also been taken to provide a contribution to venues for academic discussion. These have an associated influence on information management activity. An example is Dr. Peter Drury’s address to The Fourth International Symposium on Health Information Management Research at Sheffield in June 1999. The reality of an IM&T strategy at the local level is a much more complex issue, however. A strategy for clinical and management information systems does not exist in isolation from the past. Previous information systems, activity processes based on these and the human components of each are the legacy inherited by IM&T implementation projects. The implementation framework of Information for health looks at various means for encouraging local development issues to drive strategy. However, the new partnerships will inevitably involve a need to fuse existing systems that were developed in different environments.
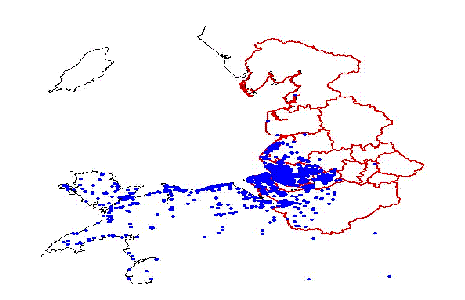
Clatterbridge Centre for Oncology (CCO) on Merseyside is the second largest centre of its type in the UK. CCO is a specialist regional centre for the treatment of malignant diseases serving a catchment population in the North West of England and North Wales. Both radiotherapy and chemotherapy modalities are provided and form the core business of the Trust. CCO has provided cancer treatment services to a wide population in Merseyside, parts of Cheshire, parts of Clwyd, Gwynedd and the Isle of Man since its establishment in 1958 and has established both national and international reputations. In terms of facilities available, the Trust is the second largest centre of its type in the United Kingdom. In terms of its geographical location, it serves a population that exhibits an especially high incidence of cancer. Figure 1 indicates the distribution of cases. The centre became an NHS Trust on 1st April 1992. Since achieving Trust status, CCO has not had a documented IM&T strategy. Contact by IM&T staff with other cancer centres and acute provider Trusts has shown the lack of a documented strategy to be exceptional.
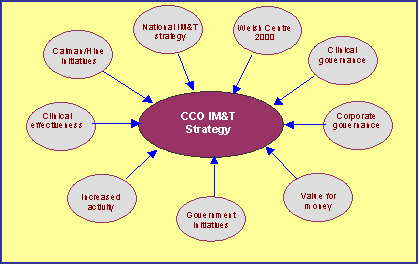
Factors that have historically and contemporarily determined the nature of oncology centres such as Clatterbridge are the background to IM&T strategy development. They appear in Figure 2. Inevitably they combine generic issues shared by all NHS organisations with issues that are specific to the unit’s place in the health market and to its clinical specialism. Some background information for each is given as a context to IM&T development.
The Calman/Hine initiatives together with the National IM&T strategy are without doubt the major drivers for the direction and implementation of all IM&T strategies for cancer centres (Calman and Hine 1995). The Calman/Hine report set out a major change in the way cancer services are delivered in the United Kingdom and as such has major implications for all Trusts providing cancer services and in particular the major regional cancer centres. Designation as a cancer centre requires accreditation, which can only be achieved if minimum standards in terms of quality and services provided are achieved. Accredited cancer centres may be actual entities providing all required facilities on a single site or ‘virtual’ centres with several establishments, each working in close collaboration. It is accepted by CCO that Calman/Hine will result in the establishment of a Merseyside Cancer Centre and that such a centre will be ‘virtual’ with CCO becoming the nucleus. Such virtual centres will require facilities to share patient based and aggregate information efficiently between the constituent cancer units and other organisations.
The number of new cancer cases is increasing for a variety of reasons and all cancer centres are facing increased activity pressures. At CCO delivery of increased activity levels, particularly in chemotherapy and the adoption of new treatment techniques in radiotherapy are expected (Millar 1999). These developments are frequently not resourced at full cost and therefore require substantial efficiency improvements in the use of staff and resources. The changes have and will continue to result in increased numbers of transactions taking place. Effective information and systems at both the operational and monitoring levels will be essential if additional costs in processing these transactions are to be avoided. Without appropriate IM&T support, acute provider Trusts including CCO will have to employ additional staff to process the paperwork or accept slippage in quality and timeliness. Cancer centres use peripheral clinics at host hospitals in order to minimise the amount of travelling required by patients to see a specialist cancer consultant. Only the initial patient attendance is recorded within the existing system and inclusion of all the activity within the Trust’s figures will involve capturing the data from some 75,000 extra transactions per year.
The concept of clinical governance was introduced in the 1997 White Paper (Department of Health 1997) and is applicable to all NHS acute provider Trusts. However, the introduction of clinical governance can only be achieved if the data required are captured and the systems are available to evaluate those data. The monitoring of clinical outcomes is complex, particularly so in the field of cancer treatments and is being addressed urgently by all cancer centres including CCO. The national minimum data set for cancer registration fails to meet the Calman/Hine requirements in terms of providing a dataset that can be used to monitor the effectiveness of cancer services (Le Maistre and Moseley 1998), a matter that needs to be addressed by a national initiative.
The assessment of internal performance will vary from Trust to Trust. Even if the response to increasing activity is discounted, CCO has a need to improve existing internal performance. Examples of current deficiencies include:
Such deficiencies are not only passed onto the service provided to patients but also create unacceptable stress levels amongst staff. Recent ‘Cancer Benchmarking Club’ data indicate that CCO is already very efficient in some areas compared to others. Therefore, the scope for improvement without major strategic and organisational change may be significantly limited compared to other Trusts.
The White Paper published in 1997 indicated a major change in commissioning with the demise of the internal market. It is as yet, unclear how the mechanisms for commissioning specialist services such as cancer treatments will work. However, it is expected that purchasers will continue to press for service monitoring to become increasingly focused on quality and outcome measures and multi-disciplinary packages of care. Such developments cannot be achieved without the use of sophisticated, integrated information systems.
The currency of contracting is forever changing, as is the basic principle of contracting itself. The Trust must be in a position to respond to whatever is required whether it is Health Resource Groups (HRG’s), ‘care packages’ or any other defined currency. The ability to respond to such a requirement is only feasible if the Trust has access to all components of care information in a quick and easy fashion.
One of the essential functions for clinical effectiveness is information (NHS Executive 1996a) and the professions have been slow to implement standards for communication and sharing information. The volume of information available can be overwhelming. Structured data collection and entry has been shown to be an effective way of providing decision support for clinical practice (Bowns 1997). The variety and complexity of clinical contexts is such that only the computerisation of clinical records and computer assisted input protocols are capable of handling the task effectively. Heightened awareness of health needs assessment has raised the profile of achieving a match between needs and outcome (Hensher and Fulop 1999).
All NHS organisations are facing financial pressures and a major aim of the national IM&T strategy is to ensure that IM&T, as with any function, must give value for money (Department of Health 1996). Installed in 1992, the principal support system (CIS/R) at CCO is unable to meet the current and future needs of the Trust. The Trust has spent approximately £250,000 in 1998/99 on its IM&T provision, which represents 1.3% of its turnover. This level of expenditure is not excessive for a NHS acute hospital but the functionality received is relatively poor when compared with the functionality and cost of modern systems.
The environmental pressures on a unit such as CCO each have their own timescale and requirements for inclusion in a local IM&T strategy. The agents that brought those pressures about were initiated by political factors and, in some cases, clinical priorities. The growing importance of medical research in an evidence-based environment gave especial importance to some of these. However, for the IM&T manager at the local level, their timing was not integrated to suit local needs, budget allocations and long-term planning. Of particular note is the fact that any local IM&T strategy devised before the change in UK government in 1997 would inevitably require substantial amendment following the publication of the White paper. For CCO and cancer centres of its kind, a strategy in accordance with the earlier Calman/Hine initiatives would need considerable revision since the necessary communication between cancer centres, units and other NHS bodies had been seen originally as being across purchaser/provider boundaries. The new national strategy inevitably needed to incorporate the requirements of government policy but also had to provide enough breadth in implementation for NHS units whose direction and timescales in IM&T were also determined by other factors. The NHS organisational structure after the internal market provides a framework that will have its own influence on the strategy’s success (Fairey 1999).
All Trusts must align themselves with the national IM&T strategy to support better care and communication through the appropriate use of IM&T (Burns 1998). These provide a more definitive (and perhaps prescriptive) framework for IM&T than the previous strategy although the basic principles remain the same (NHS Executive 1992). These are as follows.
The 1998 strategy, Information for health embodies these in the following tenets.
It is apparent from the points made above, that local IM&T strategy cannot simply be an implementation of a single set of national guidelines. Consequently CCO did not assess its information needs solely on the basis of the tenets listed, but on the pressures that clinicians and managers felt in all aspects of their work. This study outlines the findings and assesses variance from the NHS Information Authority’s guidelines. This variance could have two sources:
The major issue to be addressed by this exercise was determination of the information needed to support staff in carrying out their day to day work. This initially preceded the 1998 strategy but the analysis of the data straddled the publication of the strategy and CCO’s aim to fulfil its requirements. Failure to allow any individual or staff grouping to express their personal views and opinions would inevitably lead to non-acceptance of the final strategy document. It was also evident prior to the study that many staff had little idea of their own information needs. One senior clinician had admitted to being very embarrassed at not being able to articulate the information and functionality required to support fellow clinicians in their work. It was evident that the lack of an IM&T strategy had contributed to a very unfocused approach to identification of information needs. For these reasons the method selected to gather data on needs had to be appropriate to investigation in an environment of undirected information use. However, since staff were very conscious of their need for information, the method must produce results that were directly applicable to producing a local strategy. Abstract principles of data type, content and communication would not serve the purpose of the exercise. The size of CCO and its pre-eminence in cancer care in the north-west of the UK, made these initial soundings particularly salient. If indicative of the effect of a lack of strategy on acute providers in other specialist fields, it is unlikely that the expectations of the national strategy would be met. Consequently a fundamental survey of needs was needed. Unstructured interviews were used for senior clinicians and managers. Workshops using an unstructured questionnaire as an aide-mémoire were used to collect information from other staff. These were arranged on a discipline by discipline basis where possible. Staff had been very honest in admitting their lack of understanding with respect to information needs to the IM&T director informally. Similarly they were encouraged to be open about them within the formal study. The focus of the interviews and workshops was system functionality with respect to usefulness and effectiveness as they perceived it. The study was a snapshot of staff requirements and comprised one component of an iterative analysis process.
If local implementation of national IM&T requirements is to be successful, the determination of information requirements has to be a fundamental one, not just a symptomatic exercise in examining current problems.
For these reasons the method selected to gather this information was informal, unstructured interviews and workshops. These characteristic environments for qualitative research have a good track record (Bryman 1992). The interview and workshop topic headings were based on all known functional areas but respondents were not restricted to these headings. This method allowed the interviewer/workshop facilitator to ensure that all initially relevant points were covered whilst recognising that departures from these functional areas will occur. In this way the interviewee was permitted to think about the issues in their own way with the minimal constraint.
Bias within qualitative data collection (Selltiz et al 1962) was addressed by having a single person conduct the interviews and workshops so that while bias was not eliminated, there was an element of consistency. Although logistically difficult, the results enable case analysis to have validity. The risk of the interviewer imposing their preconceived ideas on the respondent was addressed by the unstructured nature of the interview and constant self-control on the part of the interviewer.
The views of directors, senior clinicians and senior managers were established via interviews. Workshops were arranged for all other users on the basis of disciplines. All interviews were conducted at a time and place convenient to the individual concerned, and workshops arranged with departmental managers at times most suitable to the needs of the department. The process was essentially the same for the interviews and workshops. Staff at all levels were assured that all comments and opinions were important and confidential. The approach taken was one of honesty about the purpose of the exercise, integrity in the conduct of the interview or workshop and a guarantee that all staff would have access to the completed findings as published in the final strategy document. This approach as outlined by many authors such as Judith Bell 1993) proved very effective and all the staff members involved were very co-operative and forthcoming.
Staff members were asked to consider the functionality, usefulness and effectiveness of currently used information systems, identifying the strengths and weaknesses of each as perceived by them. The results from this confirmed without any doubt the anecdotal evidence that information needs were not being met. When asked to describe their information needs in the short and long-term staff found this more difficult but the use of relevant prompts allowed a clear picture to be established for incorporation into the strategy. In addition to functionality, views were also elicited on topics such as responsibility for data capture, training in use of corporate systems, and general attitudes to IM&T in the health care setting.
The method chosen to conduct this exercise appears to have been effective from the following two distinct aspects.
Whilst the methodology chosen to carry out this exercise at CCO proved effective it cannot be argued that the issues would be equally applicable in other cancer centres. There is a need to take into account the current situation, culture, systems and organisation that exist at the time the exercise is carried out. However, CCO’s pre-eminence in its field gives the results some validity as a bench-mark.
The process of establishing the information needs requires the involvement of staff in all disciplines and at all levels. The establishment of an information management partnership between managers, end users and IM&T professionals is essential if effective information management is to be achieved (Silk 1993). The aim of the exercise as expressed by Avison (1992) is to identify and gain representation of as many views and perspectives as possible. Details of the groups identified at CCO and their associated input into the process are shown below:
Chief Executive and Executive Directors. The strategic and business context was the major focus for this group. Access was requested and given to relevant documents such as discussion papers. Directors, who had a particular lead responsibility such as finance, were also asked to express their views in that particular area.
Clinicians. In the context of this exercise, clinician is defined as any member of staff that has a clinical input into patient care. This includes nurses, radiographers and professions allied to medicine. The views of these groups in respect of information needs are of particular importance for the major strategic objective is to put in place systems that support the clinicians in their day to day work.
Senior Managers/Heads of Department. The input from this group was focused mainly on their area of responsibility such as nursing or radiology. Additional information was sought regarding information needs outside their specific area such as financial information needs for budget holders.
All other users. This group covered all disciplines and input was across all areas. This group was important as it contained the majority of end-users and was likely to be most affected by any proposed changes.
Clinicians identified the need for access to patient clinical histories and current information. The information specified is that which would create a patient based longitudinal record. The clinical staff see this longitudinal record as being necessary to support them in their day to day work and in doing so provide the means to improve quality of care. The Electronic Patient Record (EPR) is a lynch-pin of the national IM&T strategy. CCO clinicians only had a vague sense of the technological manifestation of the EPR, but its value was undeniable. The needs identified as essential in providing clinical care appear in appendix 1. In addition to these, generic needs were identified. These appear in appendix 2.
The stated resource management information requirement for CCO covers the finance and human resource services. The information needs of these appear in appendix 3. There were no surprises in this respect. The needs, particularly the financial ones, were those that would be expected within an NHS unit that must manage and refine its operational activities and also demonstrate its effectiveness in the light of the environmental factors discussed earlier. The Cancer Centre accreditation requirements of Calman-Hine signify a change in central demands which go beyond traditional formats for management reporting. A decision support function (discussed below) and decision outcome reporting had to be a core component of CCO’s IM&T strategy. The requirements of Information for health provided a general clinical motive for this, aside from those in the oncology specialism.
Senior managers provided the major input into identifying these information needs. Heads of department were particularly keen to have summary data and reports available as and when required. Appropriate information and data are required to support the following processes (Abbott et al 1996).
As stated above, decision support took on new significance with the publication of Information for health. Although CCO had found it necessary to incorporate new management information requirements following the publication of each White Paper and passing of each health service Act, managers now had an awareness of decision support that was unprecedented.
As expected the needs in this section were formulated mainly by the directors. Requirements are summarised as follows:
Many of these data were no more than those required for central returns and audit. However, the fact that the directors could readily identify specific instances of their use was an indicator of locally derived data having a heightened national status with CCO’s standing as a Cancer Centre.
Educational development was a major issue for all other users and medical clinicians. Requirements are summarised as follows:
At the time of the survey, the requirements of the new national strategy were not apparent in terms of professional development. CCO had been proactive in its own strategy with regard to the access to resources. The priority now was to place the stated requirements of staff within the context of national demands.
Staff at all levels and across all disciplines expressed their need for information that will allow them to carry out their day to day duties more efficiently and effectively. It was also made very clear that existing systems and manual processes were prohibiting staff in their desire to improve their particular area of service provision. There is evident commitment to supporting new information systems in making procedures both quicker and better. Whether it is the clinical or administrative processes involved, the end result must be improvement in the quality of care and service to the patient and their family. Although these may seem obvious goals, in information terms they pre-empted the national strategy’s aim of improving communication of data rather than refinement of internal systems. The advancement of information thinking from earlier initiatives such as the Resource Management Initiative is clear.
The results from this needs analysis confirmed without any doubt the anecdotal evidence that information needs were not being met. When asked to describe their specific information needs in the short and long-term staff found this difficult but the use of relevant prompts allowed a clear picture to be established for incorporation into the strategy. In addition to functionality, views were also elicited on topics such as responsibility for data capture, training in the use of corporate systems, and general attitudes to IM&T in the health care setting.
The perspective of the IM&T director started with the findings of the study. These defined the local needs and the impact of the environmental factors that were summarised at the start of this article. The chief obstacle, aside from resource implications of introducing a new principal information system, was the timescale of the national strategy. Its directives are well defined but traverse the situation that an individual unit such as CCO finds itself in historically. The gap of roughly 6 months between announcement of the strategy and production of the implementation plans further caused IM&T managers to postpone planning of local implementation. The lack of an existing strategy but the presence of a standing system at the core of the Trust’s information resources required strategy development that could neither wait for a national initiative, nor a timetable for the implementation of national requirements. However, if the local strategy were not in line with the national one, investment would almost certainly be lost.
The means of establishing information requirements used in this study produced a blue-print for both clinical and management information structures. Central to this was patient care which, as observed earlier, is an obvious but often overlooked priority. Previous health service initiatives have often seen optimisation of the technology as the priority, rather than outcomes of its use. Information for health and the implementation guidance that followed its publication, took a similarly patient-centred view and place the EPR at the heart of it. CCO’s strategy had a similar outcome in terms of the core information product, aiding its implementation and confirming its alignment with the national strategy. This fortuitous match can be linked to the common approach of local and national strategic policies. However, although the NHS Information Authority's current guidance is highlighting the role of co-operation between Trusts, Primary Care Groups and other health sector agencies, it is not in the form of a plan of action. This is an inevitable consequence of there being no single model for IM&T.
Findings of the sort described in this study are inevitably individual to the case and the arena in which the particular organisation operates. The discussion within this article has attempted to expand the significance of results drawn from the oncology specialism to the broader NHS arena, including the acute sector. However, the environmental factors listed involve specific elements that would not exist in a significantly different sector of health care. Nevertheless, in generalising the findings, the IM&T manager can feel secure in the certainty that the distinction between clinical, resource and activity categories of need will exist in other NHS unit types. In terms of related categories, the generalisation may be wider still. The careers of many IM&T managers started outside the health sector and their appointment within NHS bodies was often due to their ability to relate commercial and corporate information requirements and system development methods to the environment of health care. Whether the relevance for health management of equivalent information needs analysis in the commercial sector can be reversed is another matter. Much discussion of the insular nature of health sector management has taken place internationally as well as within the UK (Rondeau, K. V. and Wagar, T. H. 1999). The pace of change and the state of flux in terms of central requirements are factors that are only replicated in a small number of other business environments. Few other organisations are so constrained by requirements that have a legislative root. As such, an NHS IM&T manager moving into the commercial environment may find a need to redefine their approach to needs analysis that is greater than they would have found in moving the other way.
In terms of the NHS, however, the CCO case is replicable elsewhere. The support that the IM&T strategy achieved from clinicians and managers is indicative of the confidence that they had in the means by which their information needs were ascertained. In approving the strategy the NHS Executive has requested permission to use the CCO strategy document as an exemplar for use by other NHS Trusts starting a similar exercise.
The authors wish to thank the Chief Executive, executive directors and all staff at Clatterbridge Centre for Oncology for their co-operation during this exercise.
| Demographics | Radiotherapy planned and given |
| Patient Details | Chemotherapy planned and given |
| Name, Address, Personal details, GP Details | Care |
| Referral Information | Medical, Nursing, Physiotherapy, Dietetics, Social services, Community, Other |
| Hospital, Consultant, Date, Referred diagnosis | Diagnostics |
| Previous History | Pathology |
| Personal, familial | Requests, Results |
| Diagnostic investigations and results as relevant | Radiology |
| Assessment details | Requests, Results and images |
| Diagnosis | Other requests, Results |
| Primary tumour details, Diagnostic tests, investigations | Drugs |
| Modality | Non-Chemotherapy |
| Decision to treat date, Priority | Drugs prescribed |
| Staging | Drugs given |
| Specific staging | Clinical notes |
| Interventions | Medical, Nursing, Professions allied to medicine, Other |
| Treatment | Evaluations, Observations |
Finance This includes contracting, billing and income management. Finance staff identified their own information needs. Senior non-financial managers, particularly those who were budget holders were also requested to identify their need for financial information
Requirements are summarised as follows:
Human resources including personnel and payroll. Personnel staff and senior managers with a large staff establishment cited the following information requirements.
How to cite this paper:
Smith, Les & Preston, Hugh (2000) "Information management and technology strategy in healthcare: local timescales and national requirements." Information Research, 5(3) Available at: http://informationr.net/ir/5-3/paper74.html
© the authors, 2000. Last updated: 23rd March 2000
Contents |
|
Home |